Understanding PCOS - A Simple Model of a Common Condition
What is PCOS?
This has always been a difficult question for patients and practitioners alike, as it's such a complex condition with so much variability between patients. As a result, I’m very excited to share my simplified concept of PCOS with you all! It came to be after many years of practice and studying hormones (including metabolic hormones), integrating research from endocrinologists like Dr. Jerilynn Prior (the modern master of progesterone) at CeMCOR.
I presented this concept twice at the PCOS Awareness Symposium this weekend and will do the same at the British Columbia Naturopathic Association and Ontario Association of Naturopathic Doctors Conferences where I’m speaking this fall!
PCOS has long been one of the most challenging conditions to understand in endocrine health so I wanted to provide a simple way to show the “PCOS cycle” works and how it keeps us stuck in this pattern. Of course this is what we currently know which may adjust over time as new knowledge is added to our base.
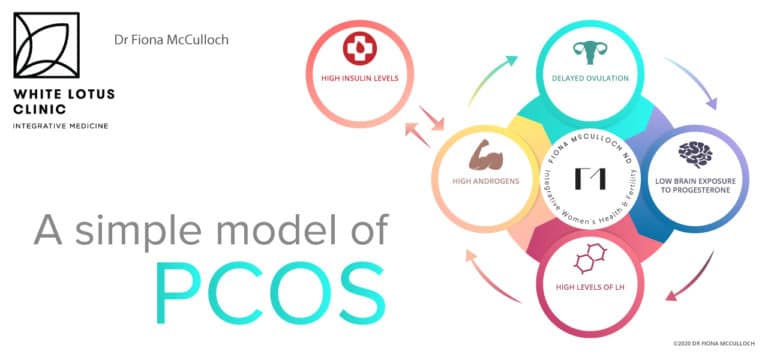
PCOS is a cycle of hormonal blockage between the ovaries and the brain
Insulin is a powerful force in perpetuating that cycle. Ultimately, insulin resistance comes from androgen excess, however it can also CREATE androgen excess.
Pathophysiology of PCOS
- High levels of androgens (ie: testosterone) within the ovary delay ovulation. This due to overactivity of the theca cells in the ovary.
- The longer the delay to ovulation, the less overall exposure the brain receives to progesterone.
- The less exposure the brain receives to progesterone, the more it engages in rapid pulsing of GnRH at the level of the hypothalamus.
- Rapid pulsing of GnRH causes high levels of LH to dominate over FSH
- LH causes the theca cells of the ovary to overproduce androgens (testosterone).
- High levels of androgens cause inflammation, fat cell dysfunction, insulin resistance, and high levels of insulin.
- High levels of insulin cause the ovarian theca cells to become overactive in their production of testosterone.
And so the PCOS cycle continues.
And yes, there are answers! To learn more, check out my book “8 Steps to Reverse Your PCOS” and/or see one of our NDs.
At our Toronto clinic our ND's treat many patients with PCOS with supplements, nutritional plans, Cyclic Progesterone Therapy and other natural therapeutics.
This diagram may be shared with attribution to Dr. Fiona McCulloch ND.