Naturopathic Endometriosis Treatment
Endometriosis is a disease defined by the presence of tissue that is similar to endometrial tissue (the lining of the uterus) .
Although menstrual pain is common in endometriosis, it involves so much more than that. Endometriosis is associated with fatigue, chronic pelvic pain, depression, anxiety, immune issues, and an increased risk of fertility concerns.
It’s symptoms can mimick irritable bowel syndrome, bladder and urinary infections, interstitial cystitis, fibromyalgia and chronic fatigue syndrome and it’s common that it is misdiagnosed as such. Due to the fact that diagnosis is made by laparoscopy (camera observation inside the abdominal cavity) and histological examination of lesions, many patients are struggling with symptoms yet are undiagnosed. Transvaginal ultrasound can often detect ovarian endometriomas (blood filled cysts — also called “chocolate cysts” present on the ovaries) but only some patients with endometriosis have these cysts. The remainder of endometriosis is invisible through ultrasound.
In recent years, the European guidelines have changed to include MRI as a diagnostic tool for endometriosis – which makes it far more accessible to patients. We are hopeful that this will allow patients to receive more clarity around their diagnosis in the future.
Although much can be done to treat endometriosis, it is still seen as a menstrual disease and the treatments offered are typically birth control pills, hormonal IUDS or medications that induce artificial menopause. With the knowledge that endometriosis is far more than a menstrual disease, we must do better and treat patients individually for the various elements of endometriosis that are impacting their lives.
Common Symptoms of Endometriosis
- Pain with or before the menstrual period
- Pelvic pain at other times of the month
- Pain with intercourse
- Pain with bowel movements/urination during menstrual periods
- Lower back pain
- Heavy or clotted periods
- Chronic fatigue
- Bloating, abdominal pain loose stools and/or constipation
- Bladder symptoms including urging, pain and sensitivity
- Depression
- Anxiety
- Sleep Disorders
- Musculoskeletal Pain
- Immune reactions and sensitivities
- Brain fog and Memory Problems
What causes endometriosis?
One longstanding theory is that backflow of menstrual blood through the fallopian tubes and into the abdominal cavity causes the onset of endometriosis. However this has been challenged, since this happens regularly during most women’s menstrual cycles and it does not cause endometriosis
However, this is seeming less and less likely as more research is completed. Although we don’t exactly know what causes endometriosis it’s thought that the most likely cause is related to the way endometrial stem cells are laid down during the formation of an embryo (yes, it seems to happen in the womb during development)
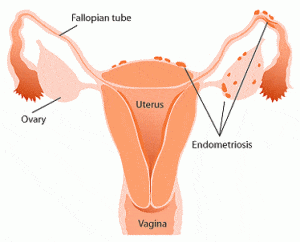
It has been found that endometrial cells can attach to and grow on the peritoneum (the lining of the abdominal wall). Endometriosis is most often found in areas near to the ovaries, between the uterus, bladder and rectum. But, it can also be found on the diaphragm, in organs like the lungs and throughout the entire abdominal cavity.
Genetic Factors in Endometriosis
Endometriosis is 6-7 times more prevalent among first degree relatives of affected women than in the general population. These genetic factors often predispose women to hormonal factors which allow the growth of endometriosis. Many women may not even be aware they have endometriosis, since there may be differing severities and since laparoscopy is often required to detect it. Often then, genetic factors for the disease do not become evident within families since many cases go undiagnosed (often simply as “painful periods”).
Hormonal Factors in Endometriosis
Related to the genetics previously discussed, some women with endometriosis have different factors that alter normal estrogen metabolism in the tissues of the endometrial lining. Some have been found to be more resistant to progesterone than others without the condition. We still have much to learn about this area.
In cases where estrogen is high – it results in local growth of the endometriosis lesions. Estradiol then stimulates a COX-2 inflammatory pathway which actually creates positive feedback for the production of even more estrogen locally in the area of the lesions. If progesterone is low, or if the person is resistant to normal amounts of progesterone (which normally opposes the effect of estrogen), this creates more opportunity for growth of the lesions.
Pain in Endometriosis
Endometriosis causes much pain for many women. It does this by causing inflammation in the peritoneal cavity, by the effect of bleeding outside the uterus, and by irritation of nerves in the pelvic floor.Even after the tissue is removed (excision) pain can persist – it’s been found that having endometriosis for years can change pain signalling and brain chemistry. This is why the management of endometriosis should be multipronged and individualized in order to address its many impacts which vary from person to person.
Infertility in Endometriosis
Endometriosis can reduce fertility in a few different ways:
- It can alter the normal anatomy of the area where the ovary meets the fallopian tube because of physical obstruction by lesions. This can make it difficult for the egg to enter the tube after ovulation.
- There are effects on the development of the egg and the embryo in endometriosis patients. This is seen when results of women undergoing IVF are considered. In women with endometriosis, there are fewer eggs retrieved, and poorer embryo development. We also often see a lower ovarian reserve in endometriosis. Since the condition is inflammatory, it causes oxidative stress that can cause damage to egg quality.
- Endometriosis can also impact implantation. This happens because the function of the endometrium in women with endometriosis is altered by inflammation.
Naturopathic Treatment of Endometriosis
In integrative naturopathic medicine there are several effective research based treatments.
Goals are to reduce growth of pathogenic tissue, manage the balance between estrogen and progesterone, reduce inflammation and pain, to enhance circulation and endometrial receptivity, and to shrink deposits of endometrial tissues when possible.
We complete a thorough assessment for chronic pain, pain-signaling, mental health, energy, sleep, digestion so we can support every element of health for patients. Most patients with endometriosis will need support in one or more of these areas.
Since every patient is different, the management of each will look different as well. There are some patients who are well-managed with comprehensive naturopathic care, (often including natural progesterone, anti-inflammatory treatments, support for stress and mental health) .
Yet, other patients do best with excision surgery for their endometriosis lesions and naturopathic care is added to conventional treatments to improve the outcome. We can support patients as they prepare for excision and provide a comprehensive naturopathic plan for recovery and healing afterwards. We can also support patients who choose or feel best with treatments like hormonal iud, birth control to minimize risks and side effect and improve the outcome.
Since endometriosis is systemic and not simply hormonal, we argue that simply suppressing the endometriosis with hormones is not enough to provide good care for the majority of patients. We are here to fill in those blanks.
References for this article:
- Speroff, Clinic Gynecologic Endocrinology and Infertility. 7th Edition 2005