Female Pattern Hair Loss and the Hair Microbiome
Women with PCOS—and around 40-50% of women, in general—will eventually develop female pattern hair loss. This is also known as Androgenetic alopecia(AGA): hair loss that’s associated with too much testosterone.
This is a multifactorial condition, as both hormones and genetics are contributing factors.
Androgens, namely testosterone and similar hormones, impact the way that hair grows. Changes in other hormones, such as fluctuating estradiol levels and progesterone reductions, can also make matters worse. These fluctuations can “uncover” underlying androgenetic alopecia.
These androgens can cause hair follicle miniaturization. Basically, they cause hairs to become smaller and thinner. They also fall out earlier, meaning they’re also shorter in length. Androgens also cause sebum to be secreted. These create an oily surface and can cause scalp “microinflammation”.
Since androgen excess is associated with other microbial imbalances (such as acne and dandruff,) a new study set out to look at the hair follicle microbiome. They focused on its role in people with androgenetic alopecia, compared to those without the condition.
Hair Follicles
Hair and skin host to different microorganisms, but most of the research done so far has been on those that inhabit human skin surface. Far less research has been on the hair follicle itself.
This study looked at hair follicles from 20 patients with AGA and controls. The researchers took samples from areas that showed evidence of miniaturization.
They discovered that hair follicles house 25% of skin microbes. Furthermore, they found that follicular glands have their own unique communities.
What They Found:
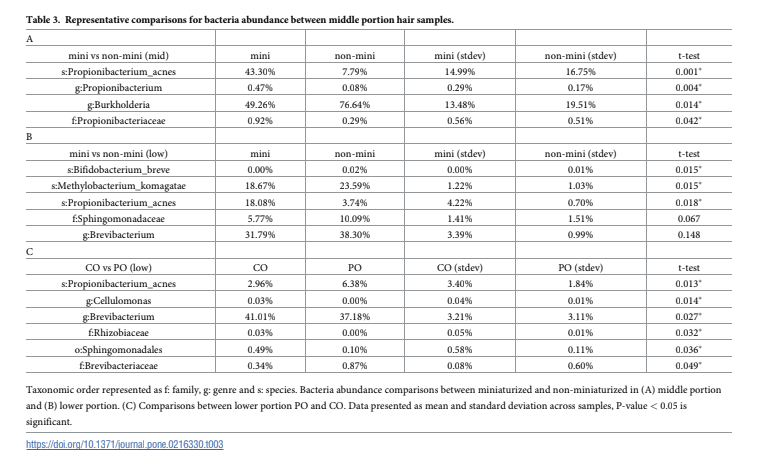
Healthy hair contains predominantly bacterial species such as burkholderia, brevibacterium, methylobacterium, and sphingomonas.
In contrast, the areas with miniaturization had an increase in P acnes—the same bacteria that is associated with acne.
Together, P acnes and the skin microflora can elicit inflammatory responses. These are similar to the microinflammation found in androgenized hair follicles. The study also found that inflammation markers from microbial response such as TLR2 were also increased in in miniaturized follicles. This corresponds with bacterial abundance in that area.
P acnes feeds off of increased levels of lipids in the skin, which occur from androgen excess creating acne.
A similar effect is found in the hair follicle: there are more fatty acids, and P acnes triggers an immune response.
This also gives us information as to why anti-microbial shampoos like Nizoral and Rosemary oil are successful in treating androgenetic alopecia.
A few of my favorite treatment options for androgenetic alopecia:
– topical melatonin spray and/or rosemary oil (diluted in a carrier)
-spearmint tea
-botanicals including white peony, licorice, pygeum, ganoderma, and saw palmetto
-supplements such as resveratrol and green tea
Also consider that hair loss is multi-factorial and many other elements can be involved including nutrient status, amino acid status, insulin resistance, inflammation, and thyroid and adrenal hormone regulation.
To learn more about PCOS-related alopecia and adrenal excess, be sure to check out these related articles:
+ Causes of Hair Loss in Women and Natural Treatments
References:
- Microbiome in the hair follicle of androgenetic alopecia patients.
Ho, Ho, Chu, Ramasamy, Bigliardi-Qi , de Sessions, Bigliardi. May 2019: https://www.ncbi.nlm.nih.gov/pubmed/31050675


