DHEA-S and Adrenal Androgens in PCOS

Written by Dr. Fiona McCulloch, ND, author of a peer-reviewed article on adrenal androgen excess in PCOS and over 25 years of clinical focus in PCOS and reproductive endocrinology.
Dr. Fiona's clinical approach to adrenal androgens in PCOS has evolved over two decades of observation as research and clinical experience have deepened understanding of the adrenal–ovarian relationship.
If your blood work came back showing elevated DHEA-S, the first thing you probably did was search for what it means. And what you found was likely some version of: “DHEA-S is an androgen produced by the adrenal glands.” That’s not wrong — but it doesn’t actually explain your result. The same DHEA-S number can mean very different things in different people, and most explanations skip the part that matters: why.
You may have already noticed this: your DHEA-S is flagged high, but your symptoms don’t quite match what you’re reading about testosterone-driven PCOS. Or maybe they do, but your testosterone is normal. Or you’ve been told it’s “adrenal PCOS” and the advice you’re finding doesn’t seem to apply. That’s not a gap in your understanding — it’s a gap in how DHEA-S is typically explained. Most sources treat it as if it were the same kind of hormone as testosterone. It isn’t — and that’s why the advice you’ve found hasn’t quite lined up.
DHEA-S is not a direct androgen — it’s an androgen precursor.
- DHEA-S can be converted into true androgens like testosterone
- DHEA-S doesn’t fit into the androgen receptor causing androgenic effects, whereas testosterone does
- DHEA-S is androgenic primarily when converted to direct androgens
In other words, DHEA-S is a raw material — not the end product. The adrenal glands are producing too much of it, but whether it actually gets converted into testosterone depends on the individual: their ovarian function, their metabolic state, their insulin levels, and factors that vary from person to person. This is why two patients with the same DHEA-S number can have completely different symptom profiles — and why a DHEA-S result, on its own, doesn’t tell you what’s actually happening.
This is also why “adrenal PCOS” is a misleading label. DHEA-S doesn’t stay in the adrenal glands — much of it is taken up by the ovaries and converted into testosterone. So even when the high number on your lab report is adrenal in origin, what it does in your body depends on the full hormonal cycle. The adrenals are the source, but the ovaries are where the impact happens.
For a detailed comparison of how these two hormones differ, see our page on how DHEA-S and testosterone differ in PCOS.
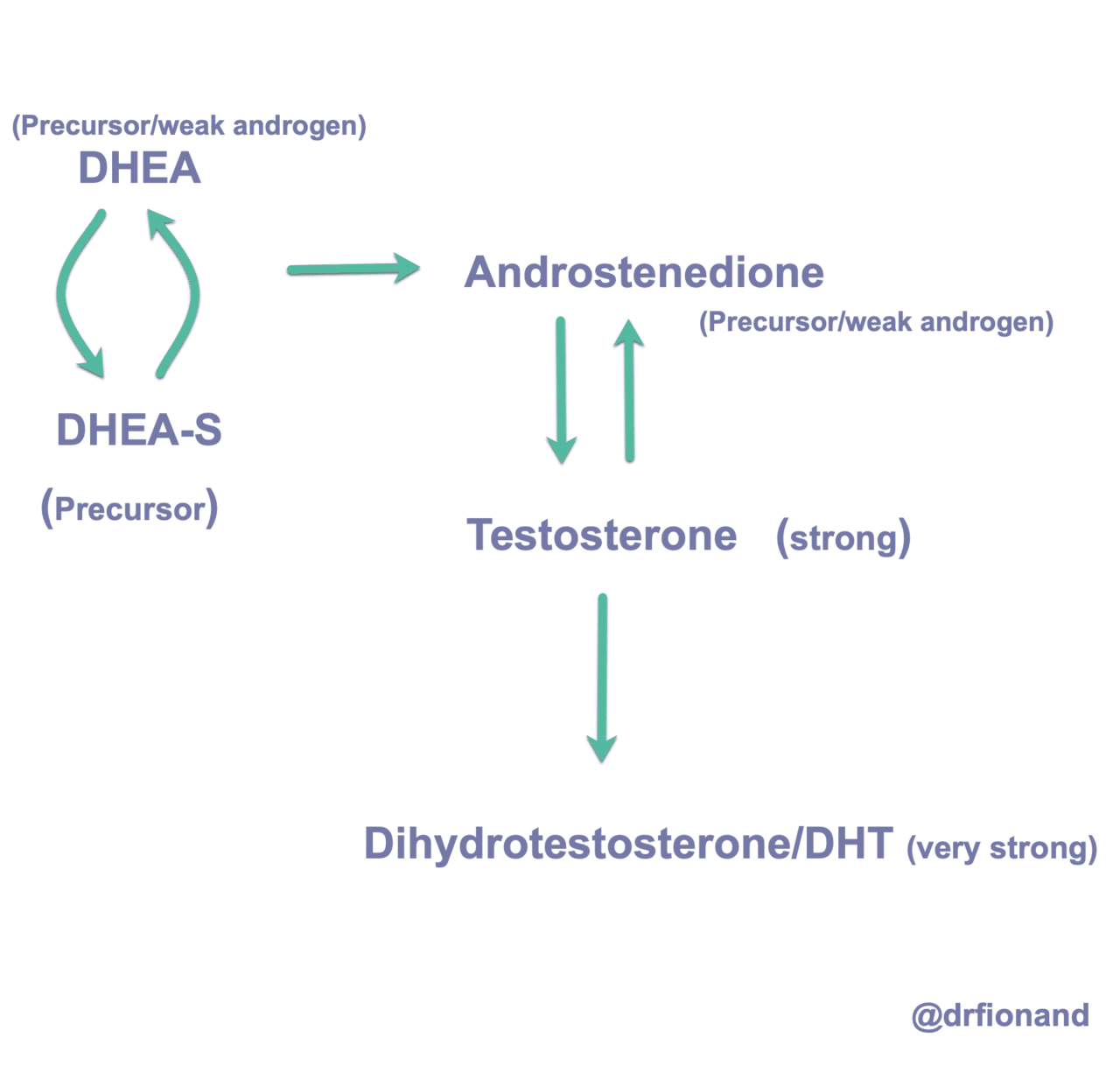

DHEA-S can follow multiple conversion pathways — which ones are active depends on the individual.
Understanding Your DHEA-S Results
Most resources stop at the definition: DHEA-S is an adrenal androgen, it’s elevated, here’s the reference range. But if you’re reading this, you’ve probably already seen that — and it didn’t resolve your question. That’s because a DHEA-S number doesn’t interpret itself. The clinical meaning depends on how elevated the level is, whether the pattern holds across repeat tests, what your testosterone and SHBG look like alongside it, and whether metabolic factors like insulin resistance are shifting how those hormones behave. There is no single reading that tells the full story — which raises the real question: how is your result actually interpreted?

Being above the reference range doesn’t, by itself, tell you how significant the elevation is — and being just inside it doesn’t mean the level is irrelevant. Mildly elevated DHEA-S is one of the most common lab findings in PCOS — so common that, on its own, it often doesn’t change the clinical picture much. Very high DHEA-S is a different situation: it may warrant investigation of the HPA axis and, in some cases, ruling out non-PCOS causes such as congenital adrenal hyperplasia or adrenal tumors. But the line between “mildly elevated” and “clinically significant” isn’t a fixed threshold — it depends on what testosterone, SHBG, and metabolic markers are doing at the same time, whether the elevation is consistent across repeat tests, and what symptoms are actually present. A single DHEA-S reading, even a high one, is the beginning of a question, not the answer to it.
What Gets Assessed Alongside DHEA-S
DHEA-S is never assessed in isolation. A comprehensive androgen assessment typically includes testosterone, DHEA-S, and, if DHEA-S is elevated, cortisol. Sex hormone binding globulin (SHBG) is also evaluated, because when SHBG is low (which is related to insulin resistance), testosterone can be more free and available in the body, potentially contributing to skin and hair symptoms even when total testosterone appears borderline.
This is one reason why insulin resistance is assessed alongside androgen levels; it can change how those androgens affect you clinically.
DHEA-S Patterns Across Age
DHEA-S naturally peaks in the mid-20s and generally declines with age, but the trajectory varies significantly from person to person. For some women, DHEA-S is always elevated. For others, it’s high only when they’re younger and gradually declines. And for some, DHEA-S rises again in perimenopause and menopause, when it needs to be considered as a potential source of androgen-driven symptoms.
Does "Adrenal PCOS" Require Different Treatment?
Many online resources describe “adrenal PCOS” as one of four distinct types, each requiring a completely different treatment approach. Clinically, this is an oversimplification. The same or similar approaches used for androgen excess generally also work for adrenal androgen excess — a pattern Dr. Fiona has observed consistently over 25 years of practice, and one that shifted her earlier view that adrenal PCOS required a fundamentally different strategy.
For most patients with mildly to moderately elevated DHEA-S, the clinical picture overlaps substantially with other forms of PCOS. The distinction becomes more meaningful only when DHEA-S is extremely high; in those cases, more targeted support for the HPA axis may be included. Adrenal-dominant patterns do tend to have less insulin resistance overall, but assessment is always individualized — no two patients receive the same plan simply because their DHEA-S is elevated.
Stress, Cortisol, and Mental Health
A common question is whether stress is driving the elevated DHEA-S. The relationship between cortisol and DHEA-S isn’t straightforward — cortisol going up is a normal part of stress physiology, and for most people with mildly elevated DHEA-S, everyday stress does not meaningfully affect their levels. But when DHEA-S is extremely high, the cortisol-DHEA axis becomes more clinically relevant, and the stress picture is assessed more carefully. The complication is that this varies: two people with the same stress history can have very different adrenal responses, influenced by genetics, metabolic state, and whether trauma or burnout is part of the picture. For some patients, mental health support becomes an important part of care — but that determination is always individualized, never assumed from the DHEA-S number alone.
What Happens to DHEA-S Levels During Treatment?
Here’s the important part. In many younger patients, after comprehensive treatment of their PCOS, testosterone and androstenedione levels decline dramatically. Yet DHEA-S levels often don’t drop to the same degree, even when the adrenals are being supported and cortisol levels have been addressed. And yet, these patients see meaningful improvements in their cycles and androgenic symptoms.
This is consistent with DHEA-S being a precursor, not a direct androgen. Even when the DHEA-S level itself doesn’t change significantly, addressing the conversion pathways (the ovarian production of testosterone from DHEA, the metabolic factors that influence that conversion, and the full cycle of PCOS) can shift the overall hormonal picture. Over more than 25 years of clinical practice, it has become clear that excluding the ovary and focusing only on the adrenals is a mistake. The entire cycle of PCOS must be treated to create a significant shift in the hormonal state.
If your DHEA-S has not declined with treatment, that doesn’t necessarily mean the approach isn’t working; it may mean that DHEA-S is behaving exactly as expected for a precursor hormone
Treatment Direction
Treatment for elevated DHEA-S involves looking at each patient comprehensively; every factor unique to their case is included. When DHEA-S is mildly elevated, the focus is typically on the underlying factors that influence whether DHEA converts into testosterone. When levels are very high, additional support for the HPA axis and stress-cortisol relationship is usually incorporated.
For Dr. Fiona’s detailed clinical article on integrative approaches for adrenal androgen excess, including the research behind specific treatment strategies; see treating adrenal androgen excess in PCOS.
Can DHEA-S Rise in Perimenopause?
In some women, DHEA-S levels rise during perimenopause and menopause, and this includes women who have never been diagnosed with PCOS before. This is a small but clinically significant group of patients who notice, often quite suddenly in their late 40s, the onset of new androgen-driven symptoms: increased facial hair (hirsutism), thinning scalp hair (androgenetic alopecia), or other skin changes that weren’t present earlier in life.
When their hormone levels are tested, elevated DHEA-S and testosterone are found; markers that may have been completely normal a few years earlier. We don’t yet fully understand why this happens. It may be genetic, stress-related, or connected to the broader hormonal shifts of perimenopause, but more research is needed.
In the assessment of women in their late 30s and 40s with these symptoms, DHEA-S is always included alongside testosterone. If DHEA-S is elevated, cortisol is assessed as well. SHBG is also evaluated, because when SHBG drops (which is related to insulin resistance and can happen as women approach menopause), more testosterone becomes free and biologically active, contributing to skin and hair changes.
If you’re noticing new hirsutism or hair changes in your late 40s and have never been told you have PCOS, you’re not imagining it, and it’s worth investigating. For more on how PCOS and perimenopause interact, see our page on PCOS and perimenopause. If you’re experiencing hormonal changes during perimenopause more broadly, our menopause and perimenopause program provides comprehensive assessment.
Common Questions About DHEA-S and PCOS
Is DHEA-S the same as testosterone?
No. DHEA-S is a precursor hormone; it can be converted into testosterone, but it doesn’t directly activate androgen receptors the way testosterone does. DHEA-S is produced primarily by the adrenal glands, while testosterone is produced mainly by the ovaries. DHEA is not as strong as testosterone; testosterone is much more powerful. They can be elevated independently of each other. For a detailed comparison, see our page on how DHEA-S and testosterone differ in PCOS.
What does it mean if my DHEA-S is high but my testosterone is normal?
This is a common pattern in PCOS. DHEA-S comes from the adrenal glands, while testosterone comes primarily from the ovaries, so they can be elevated independently. Whether DHEA-S converts into testosterone varies from person to person, depending on individual hormonal and metabolic factors. A single DHEA-S reading doesn’t tell the whole picture, which is why DHEA-S levels should be repeated a few times and assessed alongside testosterone and SHBG for a more complete understanding.
Will exercise make my DHEA-S worse?
We have not found that exercise is a problem for patients with elevated DHEA-S generally. This is a common concern, but exercise itself does not appear to raise DHEA-S levels. What we do see is that some patients, particularly those with burnout, significant stress, or insulin resistance, may find starting exercise more challenging and may have low exercise tolerance. In these cases, working up to exercise tolerance gradually tends to help. The issue is exercise tolerance, not exercise itself.
Does stress raise my DHEA-S? Should I avoid anything that raises cortisol?
For people who don’t have adrenal androgen excess, stress does not really affect DHEA-S levels, so you don’t have to be afraid of everything that might raise cortisol. Cortisol going up is completely normal and is part of healthy stress physiology. For patients who do have extremely high DHEA-S, the stress-cortisol axis may play a more significant role, and this is something that would be individually assessed. The key message: normal stress responses are not something to fear.
Is adrenal PCOS treated differently from other types of PCOS?
In many cases, adrenal PCOS is treated similarly to other forms of PCOS. The same or similar approaches used for androgen excess generally tend to work for adrenal androgen excess as well. When DHEA-S is extremely high, additional support for the hypothalamic-pituitary-adrenal axis may be included. But the idea that “adrenal PCOS” requires a completely different treatment paradigm is an oversimplification. Every case is assessed individually; treatment is always based on the full clinical picture, not on a type label.
Can DHEA-S go up for the first time in perimenopause?
Yes. Some women develop elevated DHEA-S in perimenopause, including women who have never been diagnosed with PCOS before. This typically presents as new-onset hirsutism (facial hair growth) or androgenetic alopecia (hair thinning), appearing for the first time in the late 40s. Assessment includes DHEA-S, testosterone, and SHBG. For more, see our pages on PCOS and perimenopause and our menopause and perimenopause program.
Why doesn't my DHEA-S level go down with treatment?
DHEA-S is a precursor hormone, not a direct androgen, so it may not decline to the same degree as testosterone or androstenedione during treatment. This doesn’t mean treatment isn’t working. In many patients, androgenic symptoms improve significantly even when DHEA-S remains relatively stable, because the conversion pathways and ovarian hormone production are being addressed. For a detailed discussion of treatment approaches, see treating adrenal androgen excess in PCOS.
Does high DHEA-S mean something is wrong with my adrenal glands?
Not necessarily. Mildly elevated DHEA-S is very common in PCOS and is part of the broader hormonal picture; it does not indicate a separate adrenal disease. The adrenal glands are producing more of a precursor hormone, which is typical in PCOS. However, very high DHEA-S levels do warrant further investigation to rule out other causes such as congenital adrenal hyperplasia (CAH) or adrenal tumors. Your practitioner can assess whether your levels fall within the expected range for PCOS or whether additional testing is indicated.
Assessing Your Androgen Pattern
A first visit includes a review of your androgen levels (DHEA-S, testosterone, SHBG), metabolic markers, symptoms, and history. It is exploratory — an opportunity to understand your hormonal picture, not a commitment to a treatment plan.
Learn more about our approach to comprehensive PCOS assessment in Toronto.
If your androgen symptoms are new and connected to perimenopause, our menopause and perimenopause program may be the best starting point — we assess hormonal changes comprehensively, including androgen patterns that emerge in midlife.
Consultations for PCOS Care

If your androgen symptoms are new and connected to perimenopause, our menopause and perimenopause program may be the best starting point. We assess hormonal changes comprehensively, including androgen patterns that emerge in midlife.
Related Pages
- DHEA-S vs Testosterone in PCOS — How these two androgens differ and why both are assessed
- Treating Adrenal Androgen Excess in PCOS — Dr. Fiona’s comprehensive clinical article with research references
- Androgens, DHEA, and Egg Quality — The role of DHEA and testosterone in fertility and egg quality
- PCOS Naturopath Toronto — Comprehensive PCOS assessment and care at White Lotus Clinic
- Menopause and Perimenopause Program — Hormonal assessment including androgen changes in midlife
- PCOS and Perimenopause — How PCOS and perimenopause interact


