What Is PCOS?
Whether you’re suspecting PCOS, recently diagnosed, or still trying to make sense of a diagnosis you’ve had for years, you belong here.
PCOS, short for polycystic ovary syndrome, is a common hormonal and metabolic condition that affects how the ovaries release eggs, how the body responds to insulin, and how androgens (such as testosterone) behave. It is not a single disease with a single cause. PCOS is a pattern of related changes that can show up in cycles, skin, hair, weight, mood, and fertility, at different intensities in different people. Two people with the same diagnosis can look clinically quite different.
You may be here because your period has been irregular or missing for a while, and a doctor or a search result finally put a name to it. You may have been diagnosed in your teens and never felt the explanation was complete. You may have managed PCOS for years and watched symptoms return during pregnancy, after a baby, or as perimenopause begins. You might be a partner or parent reading to understand someone you love. Wherever you are in this, the information below is written for you, not at you.
Reviewed by Dr. Fiona McCulloch, ND, author of 8 Steps to Reverse Your PCOS and peer reviewer of the 2023 International Evidence-Based PCOS Guidelines. About the author.
If You've Been Told "Just Lose Weight" Or "Your Labs Look Fine"
We completely understand, and we’ve been there with many patients. It is genuinely hard when you want to get better, you are already working on your health, and the options in front of you don’t fit. Many women who are told to “just lose weight” are already restricting calories, working out regularly, and eating better than 99% of people. They still cannot lose weight, because insulin resistance is driving the weight, not overeating. “Just lose weight” is not actionable guidance for insulin resistance. It takes specific, targeted intervention, not more effort from someone who is already doing the work.
PCOS is complicated, it intersects with metabolism, reproduction, skin, hair, mood, and long-term health, and a standard ten-minute appointment at the doctor is not structured to tease those threads apart.
What you are often looking for, if you’ve landed here, is a scope of visit including time and tools to work through each factor individually, instead of treating PCOS as one problem with one answer.
If you have tried things and they did not work, that is not final, it doesn’t mean that you can’t see improvement. More often, it means the factor that was actually driving your symptoms wasn’t the factor being treated. A comprehensive approach can make a meaningful difference, even after prior attempts.
What PCOS Actually Is: Dr. Fiona's Simplified Model
What is PCOS has always been a difficult question, for patients and for practitioners, because PCOS is genuinely complex and varies a lot between people. The simplified model I share below came out of 25 years of clinical practice and study. Its job is to make the feedback loops visible, so the place to intervene becomes clearer in each individual case.
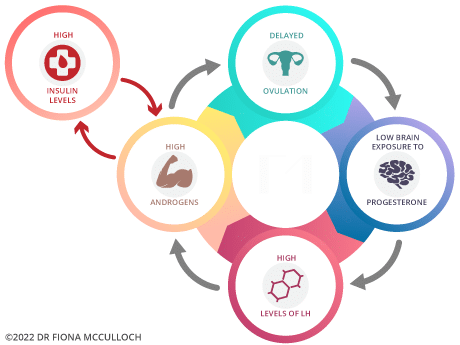
In PCOS, androgens (hormones such as testosterone) tend to run higher than expected. Androgen excess delays ovulation, and delayed ovulation means less of the body’s own progesterone. We only make progesterone for 2 weeks after ovulation.
Progesterone seems to play a more central role in PCOS than once thought. It appears to help the ovary turn over dysfunctional follicles, so when progesterone exposure is low, that clean-up step slows down and dysfunctional follicles accumulate.
Lower progesterone also changes signalling from the hypothalamus (the brain). Brain hormone (GnRH) starts pulsing more rapidly, which favours LH over FSH. LH-dominance tells the theca cells (the testosterone-producing cells in the ovary) to make more androgens. More androgens further delay ovulation, which further reduces progesterone. The cycle feeds itself.
Insulin sits on the side of this model, as a separate factor that drives the whole loop harder. Insulin resistance raises circulating insulin, and insulin directly tells the theca cells to produce even more androgens. For patients with the insulin-resistant presentation of PCOS, this input has to be addressed thoroughly, because no other intervention will hold if insulin keeps fueling the loop.
The point of this model is not that every patient needs every piece of it addressed equally. The point is that understanding which elements are most active in a given person, whether that is insulin, androgens from the ovaries, androgens from the adrenals, or progesterone exposure, is how the PCOS cycle actually gets broken clinically. That is where individualization begins.
Common Signs of PCOS
These are the signs commonly seen in clinical practice. Most people with PCOS show some of these, not all of them, and the intensity varies a lot between individuals. A single sign on its own is rarely enough to point to PCOS. What matters is the pattern across several of them.
- Irregular or absent periods. Cycles longer than 35 days, or fewer than eight to nine periods a year, are a common early clue. Ovulation often happens infrequently or not at all.
- Heavy or prolonged bleeding may occur for some patients when periods do arrive. Long gaps between ovulations can thicken the uterine lining, which can lead to heavier or longer bleeds when a period finally comes.
- Skin changes, including persistent acne along the jaw, skin tags, and patches of darkened skin on the neck, underarms, or skin folds (acanthosis nigricans). Darkened skin in particular is a visible marker of insulin resistance.
- Hair changes, including extra facial or body hair on the chin, upper lip, chest, or abdomen (hirsutism), and thinning along the hairline or crown. Both are androgen-driven.
- Difficulty losing weight despite sustained effort. Many patients report that conventional calorie and exercise strategies alone do not work, which is the hallmark of an insulin-driven pattern rather than a behaviour problem.
- Persistent fatigue in PCOS that is out of proportion to sleep, activity, or workload. It can have several overlapping drivers, including blood sugar swings, inflammation, and iron status.
- Difficulty conceiving, or irregular ovulation noticed while tracking. PCOS and fertility are closely linked, and fertility investigation is often the first context in which PCOS is diagnosed.
For the full list of signs and what each one tends to look like in practice, including the ones not covered above, see our breakdown of the 14 common signs of PCOS.
What Causes PCOS?
PCOS often involves genetic susceptibility, insulin resistance, androgen excess, and chronic low-grade inflammation. PCOS is not caused by any single thing, and in any individual patient, one or two of these factors usually carry more weight than the rest.
Genetic Susceptibility
PCOS runs in families. Large genome-wide studies continue to identify clusters of genetic variants associated with different presentations, and that research is still active. Genetics create predisposition, not inevitability. You did not cause your PCOS by something you ate, skipped, or did wrong. The genetic piece is also why reassessment later in life can matter, because the underlying predisposition does not disappear.
Insulin Resistance
Insulin resistance is present in most PCOS patients, and in many it is the central driver. It raises circulating insulin, which signals the ovaries to produce more androgens and disrupts ovulation. Insulin resistance is also one of the most difficult elements of PCOS to treat, because multiple body systems keep it in place. Testing for insulin resistance is often the first concrete step that reveals how much it is contributing.
Androgen Excess
Androgens such as testosterone and DHEA are often elevated in PCOS. The excess can come from the ovaries (ovarian androgens) or the adrenal glands (adrenal androgens). Androgen excess is what drives the skin, hair, and cycle changes most people associate with PCOS. Testing high DHEA and testosterone and understanding adrenal androgen patterns are part of working out which source is at play.
Chronic Low-Grade Inflammation
Chronic low-grade inflammation is common in PCOS and reinforces insulin resistance, so the two factors feed each other. It is not the same level of inflammation as in an obvious infection or injury. It is a quieter, measurable state that affects how cells respond to insulin and how the ovaries handle androgens. Inflammation in PCOS is often addressable through the same levers that help insulin resistance, which is part of why those two factors are worked on together.
How PCOS Can Look and Behave Differently in Different People
In clinic, PCOS rarely fits into a single clean box. Most patients show some mix of insulin resistance, androgen excess, and irregular cycles at different intensities, combined with the underlying genetic picture. Two people with the same diagnosis can present very differently and respond to very different approaches. Your job as a reader is not to work out which “type” you are and lock yourself in. It is to get a sense of which factors seem most active in your presentation, so that testing and care can be directed where they will actually move the picture.
The current scientific direction on PCOS variation is data-driven. Large clustering studies and genome-wide association research are identifying reproducible groupings of genetic variants, lab markers, and symptom patterns within tested cohorts of PCOS patients. These data-driven clusters are beginning to refine how PCOS is understood, and over time they will shape how treatment is personalized. The short version is that the science of PCOS variation is still being refined, and what we are describing in clinic is one useful working view of that variation, not the final word.
In working clinical shorthand, the common overlapping patterns we see are:
- Insulin-resistant PCOS: insulin resistance is the dominant factor, with higher fasting insulin, difficulty losing weight, and skin signs prominent.
- High-SHBG (often lean) PCOS: patients can be at a lower body weight with milder insulin resistance, but still show cycle irregularity and elevated androgens.
- High-AMH and high-LH PCOS: characterized by very high AMH and an elevated LH-to-FSH ratio, with ovulation consistently delayed or absent.
- High-androgenic PCOS: androgen excess is prominent, including adrenal androgens (DHEA-S), with skin and hair symptoms often leading the presentation.
These are not four separate categories. Most patients show features of two or more, and the mix can shift across life stages. They are working descriptions, useful for pointing testing and treatment in the right direction.
For a deeper look at how these patterns show up and what each one tends to need, see how PCOS presents differently in different people.
Why PCOS Treatment Sometimes Doesn't Work
Understanding the subtype or presentation of PCOS you have is critical, and it is the top reason people do not succeed with PCOS treatment. In clinic, we regularly see patients who have been treating insulin resistance for months or years without getting results, and when we actually look, they don’t have much insulin resistance. Their PCOS is driven by a different factor, and the treatment has been pointed in the wrong direction the whole time. Prior treatment not working almost never means PCOS is untreatable. It usually means the right factor for that individual patient had not been identified yet.
Before choosing a treatment path, the factor actually driving an individual’s PCOS has to be identified. In practice, it can include insulin resistance markers, androgen panels, AMH and LH-to-FSH, SHBG and more. How insulin resistance is tested and the full workup in the 2023 international PCOS diagnostic guidelines are a good starting place for learning more.
When the correct factor is being addressed, PCOS often responds consistently. Overall symptom improvement is often noted within six to nine months, with some elements moving on a slower schedule. If you have not seen results, the clinical question we ask first is usually not “does treatment work?” but “is the right factor being treated?” That distinction changes what to do next.
If you want to explore what factor or factors are most likely active in your case, see how PCOS presents differently in different people.
How PCOS Is Diagnosed
PCOS is diagnosed using updates from the 2023 International Evidence-Based PCOS Guidelines and the Rotterdam criteria. Two of the following three must be present:
- Irregular or absent ovulation (most commonly seen as irregular or missed periods).
- Clinical or biochemical signs of excess androgens (either visible, such as hirsutism or androgenic acne, or measurable on labs).
- Polycystic ovarian morphology on ultrasound, or elevated AMH as an accepted alternative in adults per the 2023 update.
Individual labs coming back normal or within the lab reference ranges does not rule PCOS out. PCOS diagnosis is pattern recognition across several markers and clinical signs, not a single positive test. Reference ranges are statistical averages in a general population, not optimal clinical values, and a patient can have clinically meaningful insulin resistance with fasting insulin in the upper end of “normal.”
If you have been told your labs are fine but your symptoms are telling you otherwise, the pattern is often where the answer is.
For the full diagnostic framework and the current international standard, see the 2023 international PCOS diagnostic guidelines. For the metabolic workup specifically, including what to test beyond fasting glucose, see how insulin resistance is tested.
Frequently Asked Questions About PCOS
Can PCOS be reversed?
PCOS is a lifelong predisposition, but in most cases symptoms can be reversed with the right individualized treatment. Cycles can become regular, fertility can be restored, and insulin resistance can often be reversed with consistency and the right approach for that person’s body. The predisposition itself does not disappear, and that matters practically, because insulin resistance can return at life stages that change metabolism, including pregnancy, the postpartum period, and perimenopause. At those points, the symptom picture can come back, and reassessment is worthwhile. The short answer is that PCOS does not need to be a chronic symptomatic condition, even though the underlying tendency is lifelong.
Is PCOS a lifelong condition?
Yes, the underlying predisposition is lifelong. The symptoms, however, often are not. Many patients achieve long stretches of regular cycles, resolved skin and hair symptoms, and reversed insulin resistance once the right factor is being addressed. The reason “lifelong predisposition” still matters is that it invites a maintenance view of the condition and periodic reassessment at life stages that change how the body handles insulin, rather than assuming the work is finished after the first improvement.
Can PCOS come back after pregnancy or in perimenopause?
Yes, and this is a common clinical pattern. Pregnancy induces physiological insulin resistance that can persist after delivery, and many patients notice their cycles, skin, or weight shifting in the postpartum period. Perimenopause brings its own metabolic changes that can reactivate PCOS symptoms in women whose PCOS had been well-managed for years. Neither pattern means treatment failed. It means the underlying predisposition reasserted itself under new metabolic conditions, and it is usually responsive to renewed insulin resistance management. We discuss this dynamic further in PCOS and perimenopause.
How long does PCOS treatment take to work?
Overall PCOS symptom improvement is generally expected within six to nine months when the correct factor is being treated. Some elements move faster, including cycle regularity and skin, while others, particularly insulin resistance, are slower because multiple mechanisms keep insulin resistance in place. Insulin resistance is one of the most difficult elements of PCOS to treat, and it generally needs consistent work over months, not weeks. If six to nine months pass without meaningful movement on any front, that is usually a signal to reassess which factor is actually driving the presentation, not a signal that treatment cannot work. PCOS responds consistently to the correct treatment.
Why didn't my PCOS treatment work?
The most common reason is that the treatment was addressing a factor that wasn’t the main driver in your individual case. Insulin-resistance protocols do not help someone who does not have much insulin resistance as a factor in their PCOS. This is why factor identification matters before treatment selection. See why treatment sometimes doesn’t work above for the full discussion.
Do I have PCOS if my labs are normal?
Possibly yes. PCOS is diagnosed by pattern recognition across several markers and clinical signs, not a single positive blood test. Lab reference ranges are statistical and population-based, not optimal. Fasting insulin, for instance, can sit in the upper “normal” range while being clinically meaningful for insulin resistance, especially combined with cycle irregularity or androgen-driven skin and hair symptoms. If your individual labs came back in range but your clinical picture still suggests PCOS, the next step is usually a fuller workup, including how insulin resistance is tested and the broader criteria used in the 2023 international PCOS diagnostic guidelines.
Is PCOS genetic?
PCOS has a strong genetic component and tends to run in families. Large genome-wide association studies continue to refine which clusters of variants are associated with which PCOS presentations. The key distinction is that genetics create predisposition, not determinism. Environmental and metabolic factors, especially insulin resistance, inflammation, and androgen exposure, determine whether and how the predisposition expresses. That is also why addressing those factors can reverse symptoms even though the underlying genetic picture stays the same.
At what age does PCOS start?
Symptoms often begin in adolescence, including irregular periods, acne along the jaw, and early hair changes, but many patients are not diagnosed until their twenties or thirties, often during fertility investigations. PCOS can also aggravate during perimenopause, when metabolic changes occur.
What's the difference between PCOS and PCOD?
They refer to the same underlying condition. PCOS, polycystic ovary syndrome, is the international clinical term used in current guidelines, including the 2023 International Evidence-Based PCOS Guidelines. PCOD, polycystic ovarian disease, is an older term still in use in some regions, particularly South Asia. The terminology differs, but the clinical condition is the same.
Is naturopathic care for PCOS evidence-based?
Yes. The 2023 International Evidence-Based PCOS Guidelines include lifestyle, metabolic, and pharmacological approaches that overlap substantially with naturopathic practice. Naturopathic care for PCOS draws on the same evidence base as conventional care. The distinguishing feature is not a different evidence standard. It is the time available in the visit and the scope of individualized workup, including detailed testing, nutrition, metabolism, and stress, that a standard ten-minute appointment is not structured for. Same evidence, different scope of visit.
About the Author
Dr. Fiona McCulloch, ND is the founder of White Lotus Clinic and the author of 8 Steps to Reverse Your PCOS. She served as a peer reviewer for the 2023 International Evidence-Based Guideline for the Assessment and Management of Polycystic Ovary Syndrome, the guideline that formally added AMH as a PCOS diagnostic criterion. As a legacy board member of the Endocrinology Association of Naturopathic Physicians (EndoANP), Dr. McCulloch has focused her clinical practice on PCOS and hormonal health for approximately 25 years.
An AMH number on its own tells you something, but interpreting it in the context of your age, hormonal picture, and overall health is what moves you from uncertainty to clarity. At White Lotus Clinic, that is the assessment we focus on: understanding which PCOS factors are present in your specific case and developing an approach that addresses them. If your AMH results have raised questions, a consultation at our Toronto PCOS clinic is a good next step.
Available in-person in Toronto or virtually across Ontario.


What's Next?
Three places you can go from here, depending on where you are. If you want the full list of symptoms in one place, see the 14 common signs of PCOS. If you want to understand which factors might be most active in your case, how PCOS presents differently in different people is a natural next step. And if you are considering what individualized in-person care for PCOS can actually look like in practice, here is our overview of naturopathic care for PCOS in Toronto.
References
- Teede HJ, Tay CT, Laven JJE, et al. Recommendations from the 2023 International Evidence-based Guideline for the Assessment and Management of Polycystic Ovary Syndrome. Monash University, 2023.
- McCulloch F. 8 Steps to Reverse Your PCOS. Greenleaf Book Group Press, 2016.
- Dapas M, Dunaif A. Deconstructing a syndrome: genomic insights into PCOS causal mechanisms and classification. Endocrine Reviews, 2022.

