
How to Test for Insulin Resistance
Why Standard Tests Miss It and What to Ask For
“I’ve been told that my Blood Sugar is Normal! So I’m Not Insulin Resistant, Right?”
In most medical practices, it is typical to test for blood markers of diabetes. But the majority of people with insulin resistance will test within the normal range on those standard markers. The problem is not you – it is the tests being ordered.
By Dr. Fiona McCulloch, ND, Author of 8 Steps to Reverse Your PCOS
This guide is dedicated to Dr. Joseph Kraft, MD – a pioneer in the development of insulin assays who tested 14,384 patients over his career. Dr. Kraft passed away in 2017 at age 95. His contributions to metabolic and cardiovascular health were under-appreciated in his time but have vast implications today.
Our clinic offers the advanced insulin resistance tests described in this guide, including the Insulin Glucose Challenge. If you are in Ontario and looking for accurate insulin resistance testing, we can help.
Why Standard Tests Miss Insulin Resistance
If you have been told your blood sugar is normal, yet you still experience symptoms that feel metabolic – weight that accumulates around your midsection despite effort, energy crashes after meals, skin changes you cannot explain – your experience is real. Standard fasting glucose and HbA1C tests are designed to detect diabetes, not the insulin resistance that precedes it by decades. In some patients, insulin resistance is completely invisible until a more comprehensive test is performed.
The answer is simple: the wrong tests are being recommended. The standard tests measure glucose – but insulin resistance is an insulin problem, not a glucose problem. By the time glucose levels are abnormal, insulin has often been elevated for years.
Your naturopathic doctor may recommend insulin resistance testing if you have:
- Polycystic ovary syndrome (PCOS)
- Type 2 diabetes, pre-diabetes, or a family history of diabetes
- Weight gain concentrated around the midsection
- Reactive hypoglycemia (blood sugar crashes 2-4 hours after eating)
- Fatty liver disease
- Acanthosis nigricans (dark velvety skin behind the neck or under the arms)
- Skin tags
In PCOS, women often have completely normal blood sugar levels – and can even have low blood sugar – yet their metabolisms may be significantly impaired. If you have PCOS, testing for insulin resistance is particularly important because high insulin levels drive androgen production and many of the condition’s downstream effects. Learn more about 14 signs you might have PCOS or how insulin resistance shows up as skin changes.
Insulin Resistance Is Not Diabetes - But It Can Lead There
Type 2 diabetes does not develop overnight. It begins with insulin resistance, often starting decades before blood sugar levels become abnormal. As cells become less sensitive to insulin’s message, the pancreas produces increasingly higher amounts of insulin to manage blood sugar. This means blood sugar can remain normal for years – even as insulin levels climb to levels that damage the cardiovascular system, disrupt hormone balance, and impair metabolism. The condition is called hyperinsulinemia: higher-than-normal insulin, with normal-looking glucose.
How to Test for Insulin Resistance: Every Test Compared
Here are the most commonly completed tests for metabolic health. Many of these will not pick up insulin resistance – but understanding the background helps you know which tests to request and why.

Fasting Glucose
A simple test of blood sugar measured after an overnight fast, fasting glucose is particularly good at detecting diabetes. Levels above 5.5 mmol/L (99 mg/dL) indicate a higher chance of diabetes. However, many individuals with normal fasting glucose have significant insulin resistance; because this test measures glucose, not insulin. It cannot tell you how hard your pancreas is working to keep that glucose level normal.
HbA1C
HbA1C approximates your average blood sugar over the past 2-3 months by measuring the percentage of hemoglobin with sugar attached. An HbA1C between 5.6% and 6.4% indicates pre-diabetes; above 6.5% indicates likely diabetes. While this provides useful information on glucose control, it is still a glucose test – not an insulin test. It cannot detect the elevated insulin that characterizes early insulin resistance. It is also important to note that iron deficiency anemia can cause falsely elevated HbA1C levels.
Oral Glucose Tolerance Test (OGTT)
For this test, patients fast overnight, then drink a glucose solution while blood sugar is measured at intervals over two hours. Blood sugars under 7.8 mmol/L (140 mg/dL) are considered normal; over 11.1 mmol/L (200 mg/dL) indicates diabetes. Yet again, this test measures glucose only. Many patients with significant insulin resistance will have completely normal glucose tolerance tests. Passing this test does not mean your metabolism is healthy – it only means your pancreas is still producing enough insulin to compensate.
The majority of those who have metabolic problems and insulin resistance will test within the normal range for all of the above markers.
Fasting Insulin
Fasting insulin directly measures insulin levels after an overnight fast. It is relatively inexpensive and easily accessed, but unfortunately it is not often ordered by physicians. Patients with moderate or severe insulin resistance will often have an elevated fasting insulin level. According to the NHANES III Survey, the average fasting insulin level is approximately 8.8 uIU/mL for men and 8.4 uIU/mL for women (Harris et al., 2002).
Although fasting insulin is a good screening test for severe insulin resistance, it often cannot pick up moderate or mild insulin resistance – because some patients have normal fasting insulin but produce dramatically elevated insulin after eating.
| Measure | uIU/mL | pmol/L | Interpretation |
|---|---|---|---|
| Population average (female) | ~8.4 | ~58 | Reference baseline (NHANES III) |
| Optimal range | <10 | <69 | Lower risk of metabolic disruption |
| Elevated | >12 | >83 | Suggests insulin resistance — further testing recommended |
HOMA-IR (Homeostatic Model Assessment)
HOMA-IR is a mathematical calculation based on the ratio between fasting insulin and fasting glucose. It provides an approximation of insulin resistance and correlates well with the euglycemic clamp method – a research gold-standard that is not practical for clinical use. To calculate HOMA-IR, you need your fasting glucose and fasting insulin values. The Oxford HOMA calculator is freely availabl
| HOMA-IR Score | Interpretation |
|---|---|
| Under 1.5 | Metabolically healthy |
| 1.5 – 2.0 | Mild insulin resistance |
| Above 2.0 | Moderate to significant insulin resistance |
While HOMA-IR is a useful and accessible calculation, it is still based on fasting values alone. It cannot detect the post-meal insulin patterns that a glucose challenge test reveals.
C-Peptide
C-peptide is a molecule linked to insulin when it is first produced, making it a marker of endogenous insulin production. It is not often tested except in suspected type 1 diabetes, but fasting levels above the normal range (0.51–2.72 ng/mL) can also serve as a surrogate marker of insulin resistance.
Triglycerides
Of the lipid panel, triglycerides are the most specific marker for insulin resistance. When the liver has more energy stored than it needs, additional glucose is converted into fatty acids that become triglycerides. Insulin inhibits the breakdown of triglycerides from fat cells, so insulin resistance is linked with their accumulation. High triglycerides alongside other metabolic markers can support an insulin resistance assessment.
| Level | mg/dL | mmol/L |
|---|---|---|
| Normal | Less than 150 | Less than 1.7 |
| Borderline high | 150–199 | 1.8–2.2 |
| High | 200–499 | 2.3–5.6 |
| Very high | 500+ | 5.7+ |
Waist-to-Height Ratio: A Free Self-Assessment
A completely free yet accurate marker of insulin resistance is the waist-to-height ratio – your waist circumference divided by your height in the same units. A 2010 study following 11,000 subjects for 8 years found that waist-to-height ratio was a better predictor of heart attack, stroke, or death than BMI (Schneider et al., 2010). A 2016 study of 754 reproductive-age women found it was a good predictor of insulin resistance and metabolic syndrome in women with and without PCOS (Behboudi-Gandevani et al., 2016). Ratios over 0.5 are considered high risk for metabolic health. This is a useful first screen you can do at home – though it cannot replace laboratory testing, which measures actual insulin levels.
The Insulin Glucose Challenge: The Most Accurate Test for Insulin Resistance

By far, the most valuable test for insulin resistance, hyperinsulinemia, and other blood sugar dysregulations is the insulin assay with oral glucose tolerance test. We frequently order this test at our clinic – we call it the Insulin Glucose Challenge in our practice.
Dr. Joseph Kraft was a pathologist who completed over 3,000 autopsies and found atherosclerosis in every person over 40, at which point he became interested in how this developed. He found that the slow development of atherosclerosis was linked primarily to insulin resistance and hyperinsulinemia. Dr. Kraft ran the insulin assay with oral glucose tolerance test on 14,384 patients and published his groundbreaking results – data we can use today to understand metabolic health decades before diabetes develops.
This test uses the same glucose tolerance test infrastructure as standard medical practice – the only difference is that insulin is measured alongside glucose at each interval. It is not an alternative or experimental procedure. It is, however, an under-researched test: formal academic research has not kept pace with its clinical utility, and it deserves wider adoption.
How Does the Insulin Glucose Challenge Work?
The patient fasts overnight and then completes fasting blood work. A glucose solution is consumed, and at each interval during the 2- or 4-hour test, insulin is measured along with glucose. This provides insight into patterns of insulin resistance that fasting tests alone cannot reveal. Not only are fasting levels checked, but increases in insulin production when stimulated by glucose become clearly visible.
The Insulin Glucose Challenge is particularly useful for patients who want a detailed picture of their insulin dynamics, who have unclear patterns of insulin resistance, or whose fasting levels appear normal. It is also valuable for reactive hypoglycemia – severe drops in blood sugar 2-4 hours after eating – as the test reveals the insulin dynamics that cause these crashes. A phenomenon called gastric dumping, another cause of reactive hypoglycemia, can also be identified through the specific patterns in insulin release and glucose levels.
The Kraft Insulin Patterns: Stages of Insulin Resistance
(Reference: J. R. Kraft, 2011)
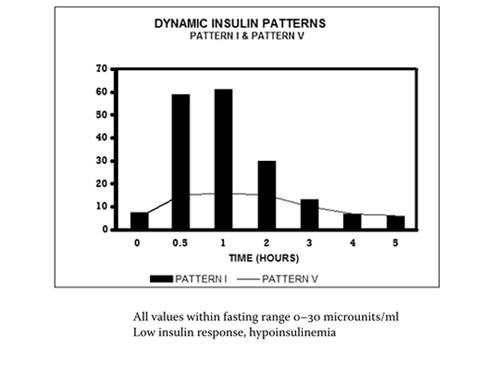
Pattern 1 represents normal insulin signaling. Note the quick rise to maximum insulin at 0.5 to 1 hour after consumption of the glucose beverage. Insulin levels then quickly drop back down to fasting levels. This is what a healthy insulin response looks like.
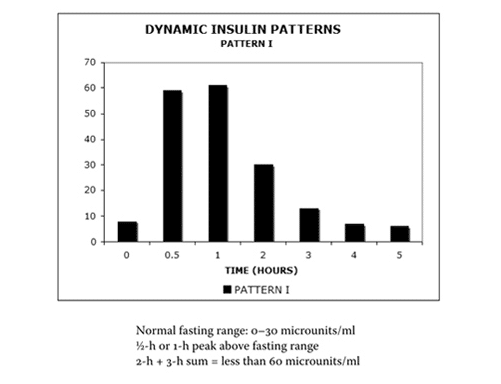
Pattern 2 represents hyperinsulinemia. The overall levels of insulin secreted are far higher than in Pattern 1, with a prominent peak at 1 hour and a striking delay in returning to fasting levels. In clinical practice, this pattern of prolonged high insulin levels is commonly seen in patients with fatty liver disease – the insulin stays elevated for longer than it should, reflecting deeper metabolic disruption.
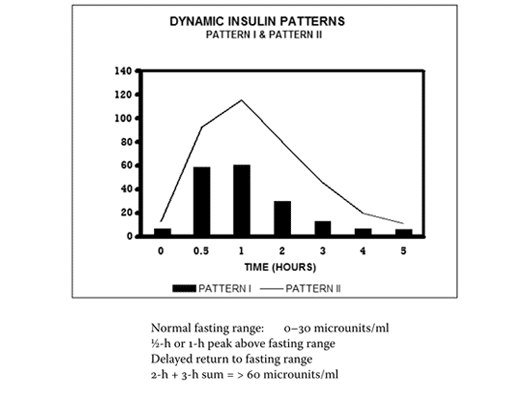
Pattern 3 also represents hyperinsulinemia, but more marked than Pattern 2. There is a striking peak in insulin by 2-3 hours. Often in these patients, there is also impaired glucose tolerance during the test – meaning blood glucose itself begins to rise, indicating the pancreas can no longer fully compensate.
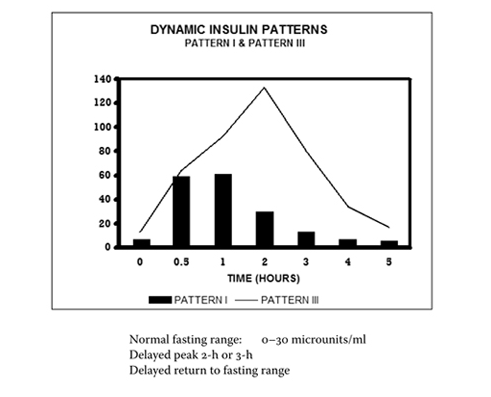
Pattern 4 includes hyperinsulinemia with impaired glucose tolerance. The insulin levels here are exceptionally high, with a 2-3 hour sum of insulin over 320 microunits/mL (1,920 pmol/L). This pattern indicates significant insulin resistance alongside glucose dysregulation.
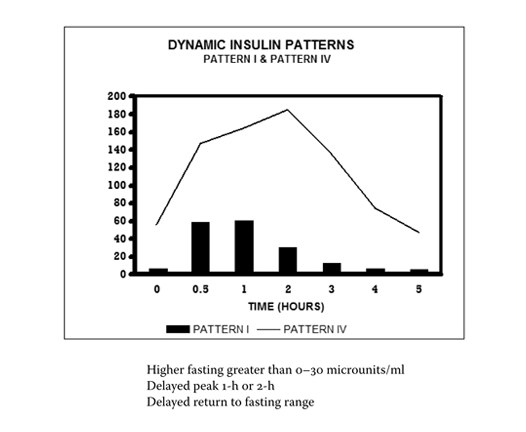
Pattern 5 represents hypoinsulinemia, often with impaired glucose tolerance. This pattern occurs when the pancreas can no longer produce adequate insulin – it is seen just prior to the development of autoimmune type 1 diabetes.
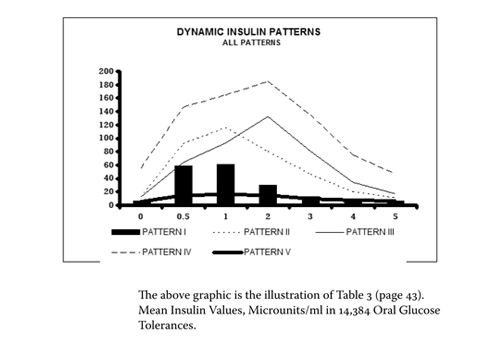
This summary overlay shows all insulin patterns superimposed, highlighting the striking differences in insulin release between the normal pattern and the hyperinsulinemic patterns. Patterns 2 through 4 would all be invisible on a standard fasting glucose or fasting insulin test.
We offer the Insulin Glucose Challenge at our Toronto clinic. This is the same test described above — a glucose tolerance test with insulin measured at each interval. Your naturopathic doctor reviews your results, explains your specific insulin pattern, and works with you to create a plan based on what the test reveals. Book a consultation.
What Happens When You Come In for Insulin Resistance Testing
1
Case review
Your naturopathic doctor reviews your full health history, symptoms, and any previous testing. This detailed conversation is the foundation of accurate assessment - it determines which tests will be most informative for your individual situation.
2
Clinical assessment.
Based on your history and symptoms, your ND selects the appropriate tests. For patients who want a deep dive into their insulin dynamics, or whose fasting levels appear normal, the Insulin Glucose Challenge is typically recommended. For a simpler screen, a fasting insulin with HOMA-IR calculation may be sufficient.
3
Test ordering
A comprehensive insulin resistance panel typically includes: the Insulin Glucose Challenge (or HOMA-IR), along with HbA1c, a lipid panel, liver enzymes, and hs-CRP. These companion tests assess related metabolic markers - lipid health, liver function, and systemic inflammation - that are important for the complete clinical picture.
4
Results review
Your naturopathic doctor reviews the results with you, explains your insulin pattern, and creates a personalized plan based on what the testing reveals. Clinical interpretation is part of the service - you are not left with a lab printout to decipher on your own.
Whatever the testing reveals, there is always a path to significant improvement with insulin resistance. When deeper insulin resistance is identified, it may require a longer or more intensive treatment approach – but the path forward exists. Treatment approaches are individualized and may include lifestyle modifications, targeted nutrition strategies, and evidence-based supplements, tailored to your specific pattern and health picture.
Ontario naturopathic doctors have prescribing and laboratory-ordering authority. All tests described on this page are standard laboratory tests processed by accredited laboratories. Results are valid medical documents – many patients share them with their family doctor as part of their overall care. Naturopathic assessment is complementary to the care you receive from your GP, not a replacement for it.
Frequently Asked Questions About Insulin Resistance Testing
Can you test for insulin resistance at home?
Yes – the waist-to-height ratio is a free, validated marker. Measure your waist circumference and divide by your height in the same units. Ratios over 0.5 indicate elevated metabolic risk. An 11,000-person study found this measure was a better predictor of cardiovascular events than BMI (Schneider et al., 2010). However, a waist measurement cannot replace laboratory testing, which measures actual insulin levels. The waist-to-height ratio is a useful first screen; clinical testing provides a definitive picture.
What blood test shows insulin resistance?
The most accurate single blood test is the Insulin Glucose Challenge (Kraft protocol), which measures insulin alongside glucose over 2-4 hours. Other useful tests include fasting insulin, HOMA-IR calculation, HbA1C, and a lipid panel. Standard fasting glucose alone misses most insulin resistance – it measures glucose, not insulin. See the full test comparison above for the strengths and limitations of each.
Can a naturopathic doctor order insulin resistance tests in Ontario?
Yes. Ontario naturopathic doctors have laboratory-ordering authority and can order all the tests described on this page, including the Insulin Glucose Challenge. Tests are processed by accredited laboratories, and results are valid medical documents that can be shared with your family doctor.
How much does insulin resistance testing cost?
Initial consultations include a comprehensive case review and test-ordering. Lab tests are often covered by extended health benefits through employer insurance plans. Naturopathic visits are covered by most extended health plans in Ontario. See our hours and fees page for current consultation rates. We are happy to discuss costs before your first visit.
Is the Kraft test (Insulin Glucose Challenge) a recognized medical test?
Yes. The Insulin Glucose Challenge uses the same glucose tolerance test procedure as standard medical practice – the only addition is that insulin is measured alongside glucose at each interval. It was developed by Dr. Joseph Kraft, a pathologist, based on research involving 14,384 patients. The test uses standard laboratory equipment and accredited labs. It is an under-researched test – formal academic research has not matched its clinical utility – but it is not alternative or experimental. It is standard medicine with one extra measurement.
How long does the Insulin Glucose Challenge take?
The test takes 2-4 hours, depending on the protocol your naturopathic doctor recommends. It is typically a morning appointment because of the overnight fasting requirement. The process involves a fasting blood draw, then a glucose drink, followed by blood draws at regular intervals. It is one morning for a detailed picture of your insulin dynamics – information that fasting tests simply cannot provide.
Will my family doctor accept results from a naturopathic clinic?
These are standard laboratory tests processed by accredited laboratories. Results are presented as formal lab reports – the same format your family doctor receives from any laboratory. Many patients share their results with their GP as part of their overall care. Naturopathic assessment is complementary to conventional medical care, and the lab data is the same regardless of who ordered it.
What is a normal fasting insulin level?
The NHANES III population average is approximately 8.4-8.8 uIU/mL (58-61 pmol/L). However, “normal” on a lab report does not necessarily mean optimal. A fasting insulin in the upper end of the standard reference range may still indicate early insulin resistance – because fasting levels can appear normal while post-meal insulin is dramatically elevated. This is precisely why the Insulin Glucose Challenge provides more information than a fasting test alone.
What is a good HOMA-IR score?
A HOMA-IR score under 1.5 is generally considered metabolically healthy. Scores between 1.5 and 2.0 suggest mild insulin resistance. Scores above 2.0 indicate moderate to significant insulin resistance. HOMA-IR is calculated from your fasting insulin and fasting glucose – the Oxford HOMA calculator is freely available. Keep in mind that HOMA-IR is based on fasting values only and cannot detect post-meal insulin patterns.
Is this test useful for reactive hypoglycemia?
Yes. Reactive hypoglycemia – blood sugar crashes 2-4 hours after eating – is one of the clinical indications for the Insulin Glucose Challenge. The test reveals the insulin dynamics causing these crashes: patterns of exaggerated insulin release that drive blood sugar down too quickly. It can also identify a phenomenon called gastric dumping. If you experience blood sugar crashes after meals that your doctor has not been able to explain, this test can provide answers.
If the test shows insulin resistance, does that mean I am pre-diabetic?
Insulin resistance is not a diabetes diagnosis. It is a metabolic pattern that can develop decades before blood sugar becomes abnormal. Identifying it early is the point – it means there is time to address it effectively. There is always a path to significant improvement with insulin resistance, including lifestyle modifications, targeted nutrition, and evidence-based supplements tailored to the individual. Finding insulin resistance on a test is not a sentence – it is an opportunity to intervene while the window for change is widest.
Can my GP order these tests, or do I need a naturopath?
Your family doctor can order fasting insulin and calculate HOMA-IR – and if they are willing, that is a good starting point. The Insulin Glucose Challenge – which involves measuring insulin at multiple intervals over 2-4 hours – is less commonly ordered in standard medical practice. If your GP does not offer it, a naturopathic doctor with laboratory-ordering authority in Ontario can. Both paths give you useful information; the Insulin Glucose Challenge provides the most detailed picture.
Getting Tested for Insulin Resistance in Canada
In Canada, fasting glucose and HbA1C are routinely ordered by family doctors. Fasting insulin and HOMA-IR are available but less commonly ordered. The Insulin Glucose Challenge – which measures insulin at multiple intervals over 2-4 hours – is rarely ordered in standard practice, despite being the most informative test for detecting early insulin resistance. Ontario naturopathic doctors can order all of these tests through accredited laboratories.
At White Lotus Clinic in Toronto, we routinely order comprehensive insulin resistance testing as part of our metabolic health assessments. Available tests include:
- Insulin Glucose Challenge (the Kraft protocol described in this guide)
- Fasting insulin with HOMA-IR calculation
- HbA1c
- Lipid panel
- Liver enzymes (ALT)
- hs-CRP (high-sensitivity C-reactive protein)
Book an insulin resistance assessment. Your first visit includes a comprehensive case review and personalized testing plan. Virtual consultations are available for the initial assessment – lab work is completed at an accredited laboratory near you. Book a consultation.
Why Early Testing Matters: What Insulin Resistance Does Over Time
When insulin resistance is identified early – even when fasting levels appear completely normal – there is always a path to significant improvement. Treatment approaches that combine lifestyle modifications, targeted nutrition, and evidence-based supplements can meaningfully change the metabolic picture. The earlier insulin resistance is found, the more options are available and the more responsive it tends to be.
The clinical evidence for why early testing matters is sobering. The very first effect of hyperinsulinemia is pathology of the arterial wall – chronic exposure to high insulin levels promotes the development of early atherosclerosis (Stout, 1979). It is known that retinopathy, which involves changes to blood vessels in the eye, develops at least 7 years before diabetes is clinically diagnosed (Harris et al., 1992). And up to 80% of type 2 diabetics die from cardiovascular complications (Reasner, 2008). These statistics describe what happens when insulin resistance goes undetected for decades. They are the reason that testing – early, accurate testing – changes the trajectory.
Once insulin resistance is identified, your naturopathic doctor works with you on an individualized plan that may include:
Meet our medical director, Dr Fiona Mcculloch, ND
Dr. Fiona McCulloch is the founder and medical director of White Lotus Clinic, where she has practiced naturopathic medicine with a clinical focus on hormonal and metabolic health for over 25 years.
- Fellow of the American Board of Naturopathic Endocrinology
- Author of 8 Steps to Reverse Your PCOS
- Peer reviewer, 2023 International Evidence-Based PCOS Guidelines
- Board member, Endocrinology Association of Naturopathic Physicians (EndoANP)
White Lotus Clinic – Est. 2002, Toronto.

Ready to Get Accurate Insulin Resistance Testing?
You now understand why standard blood sugar tests miss insulin resistance and which tests provide the complete picture. Our naturopathic doctors routinely order the Insulin Glucose Challenge and comprehensive metabolic panels – it is a core part of what we assess. If you would like to discuss whether this testing is right for your situation, we are here to help.
Virtual consultations are available for your initial assessment. Lab work is completed at an accredited laboratory near you.
References
- Behboudi-Gandevani, S., Ramezani Tehrani, F., Cheraghi, L., & Azizi, F. (2016). Could “a body shape index” and “waist to height ratio” predict insulin resistance and metabolic syndrome in polycystic ovary syndrome? European Journal of Obstetrics & Gynecology and Reproductive Biology, 205, 110-114.
- Harris, M. I., Cowie, C. C., Gu, K., Francis, M. E., Flegal, K., & Eberhardt, M. S. (2002). Higher fasting insulin but lower fasting C-peptide levels in African-Americans in the US population. Diabetes/Metabolism Research and Reviews, 18(2), 149-155.
- Harris, M. I., Klein, R., Welborn, T. A., & Knuiman, M. W. (1992). Onset of NIDDM occurs at least 4-7 yr before clinical diagnosis. Diabetes Care, 15(7), 815-819.
- Kraft, J. R. (2011). Diabetes Epidemic & You: Should Everyone Be Tested? Trafford Publishing.
- Kraft, J. R., & Noller, K. T. S. (1993). Fasting Hyperinsulinemia: Diagnostic Parameters Applicable to Neurootological Equilibriometric and Related Metabolic Disorders. Proceedings of the NES, Volume XXI, 303-307.
- Mumm, H., Altinok, M. L., Henriksen, J. E., Ravn, P., Glintborg, D., & Andersen, M. (2016). Prevalence and possible mechanisms of reactive hypoglycemia in polycystic ovary syndrome. Human Reproduction, 31(5), 1105-1112.
- Reasner, C. A. (2008). Reducing Cardiovascular Complications of Type 2 Diabetes by Targeting Multiple Risk Factors. Journal of Cardiovascular Pharmacology, 52(2), 136-144.
- Schneider, H. J., Friedrich, N., Klotsche, J., et al. (2010). The Predictive Value of Different Measures of Obesity for Incident Cardiovascular Events and Mortality. The Journal of Clinical Endocrinology & Metabolism, 95(4), 1777-1785.
- Stout, R. W. (1979). Diabetes and atherosclerosis – The role of insulin. Diabetologia, 16(3), 141-150.


