The Benefits of Cyclic Progesterone Therapy
What is Progesterone?
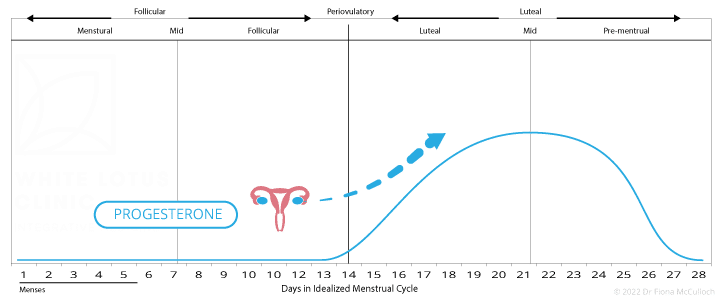
Progesterone is the natural hormone released by the ovary, after ovulation occurs. Levels of progesterone are high for approximately two weeks after ovulation, after which they drop to a low level, inducing the next period.
Progesterone is a natural hormone and is different from synthetic PROGESTINS, which are commonly prescribed in birth control pills, hormonal IUDs or in other similar medications. Synthetic progestins have more risks and don’t provide the same benefits as natural progesterone.
Despite research confirming the clear differences between progesterone and progestins, it’s still common for practitioners to think of them as the same.
Natural progesterone acts as a natural anti-androgen, reduces levels of LH and is an important factor in the communication between the brain and ovary in the process of healthy ovulation.
Symptoms of Low Progesterone
If progesterone is too low it can cause
- Heavy periods
- Painful Periods
- In patients with PCOS and excess of testosterone: unwanted hair growth, androgenetic hair loss, irregular cycles
- Premenstrual syndrome
- In perimenopause: insomnia, irritability and anxiety
- Fertility concerns like miscarriages or implantation failure
- Inflammation (progesterone is anti-inflammatory)
What is Cyclic Progesterone Therapy
Cyclic progesterone therapy involves taking natural progesterone at bedtime for 2 weeks “off” and 2 weeks “on” every month. This follows the natural pattern of hormone production and can help reestablish normal hormonal balance. At the end of the 2 weeks “on” patients will typically have a menstrual bleed and the cycle begins again.
Cyclic progesterone therapy is generally given for a minimum of 3 months and in many cases for longer.
In our Toronto clinic, our naturopaths prescribe cyclic progesterone in the form of natural micronized progesterone suppositories.
The approach to cyclic progesterone therapy varies depending on your condition, life stage, and whether you are currently ovulating. Below, we describe how it applies to specific conditions. Further down, we explain how cyclic compares to continuous progesterone therapy and what factors guide that clinical decision.
Cyclic Progesterone and PCOS
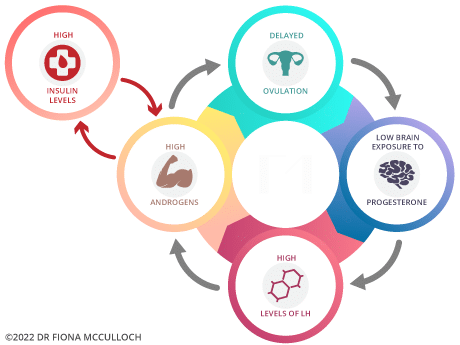
Cyclic progesterone therapy works at the level of the brain in PCOS, to help manage levels of testosterone and androgens.
Women with PCOS often have low levels of progesterone as they do not ovulate regularly, and therefore don’t make enough of this hormone. Cyclic progesterone therapy reduces levels of LH by slowing the pulsation of GNRH(1), hormones produced by the brain that regulates how the ovary makes hormones.
When repeated in consecutive cycles at the correct dose, most patients experience a reduction in LH and androgens or testosterone levels along with their androgenic symptoms of PCOS.
Since androgens like testosterone are often involved in blocking ovulation, many PCOS patients begin to ovulate with this treatment.
Progesterone can also prevent endometrial hyperplasia and atypia as it induces withdrawal bleeds.
The most common prescription to induce withdrawal bleeds in PCOS is NOT natural progesterone it is actually a synthetic progestin: medroxyprogesterone commercially known as Provera. Withdrawal bleeds can also be achieved with natural cyclic progesterone.
Since androgen excess is the underlying cause of insulin resistance in PCOS, cyclic progesterone can also support the management of insulin resistance and a healthy metabolic rate.
Cyclic Progesterone in Perimenopause and Menopause
Cyclic progesterone therapy has many applications for perimenopause. It can lighten the problematic heavy menstrual cycles that are common in this phase of life. It can support deeper sleep and help to manage mood, anxiety and irritability.
Cyclic progesterone is generally continued until cycles become extremely irregular or cease. At that point, the choice between cyclic and continuous progesterone becomes more individualized. We start from clinical experience, knowing which regimens tend to work well, and then customize based on how each patient responds. Some patients feel better with the rhythm of cycling on and off; others prefer the consistency of continuous use. There is no single correct approach — the goal is to find the regimen best suited to you.
In perimenopause, the ovaries are still producing significant amounts of estrogen — often more than usual — while progesterone production becomes increasingly inconsistent. This is why cyclic progesterone is typically the approach used during this phase: if progesterone is given continuously while a woman still has any regularity to her cycle, it can actually make cycles more irregular rather than less.
For patients in perimenopause experiencing sleep disruption, cyclic progesterone may also support deeper rest through its calming effects on the nervous system. Learn more about progesterone for sleep in perimenopause. If you are looking for comprehensive care during this transition, explore our menopause and perimenopause program.
In menopause, cyclic progesterone therapy can improve:
- bone density
- sleep
- mood
- hot flashes

Cyclic Progesterone for Heavy or Painful Periods
One of the most consistent benefits of cyclic progesterone therapy is that it can lighten heavy periods also known as menorrhagia. Progesterone opposes the effect of estrogen on the lining, keeping it in check and reducing heavy bleeds.
For a more detailed discussion of how progesterone can be used specifically for menstrual bleeding, see our article on progesterone for heavy menstrual bleeding.
Cyclic Progesterone for Endometriosis
Endometriosis is a whole-body inflammatory condition where cells similar to those which line the uterus are found in different locations in the body. Patients with endometriosis can have a variety of symptoms including fatigue, menstrual pain, painful intercourse, and bowel symptoms just to name a few. Due to its antiinflammatory effects, cyclic progesterone therapy can support many of the symptoms of endometriosis and may reduce the excessive overgrowth of these cells(3).
We have found that many patients seeing us for endometriosis treatment in our Toronto clinic improve with cyclic progesterone therapy.

Cyclic Progesterone for Endometriosis
Progesterone is required to support the implantation of an embryo within the endometrial lining. Low levels of progesterone have been linked to miscarriages. Progesterone exerts anti-inflammatory effects which are likely crucial for healthy implantation and pregnancy(4). Progesterone may be more important for patients with inflammatory or autoimmune conditions who are trying to conceive.
When given for fertility, cyclic progesterone is given after ovulation as a vaginal suppository for 2 weeks out of every cycle. If a patient is not ovulating regularly, has PCOS and is trying to conceive, progesterone is given for 2 weeks “on” and 2 weeks “off”
Cyclic vs. Continuous Progesterone: When Is Each Approach Used?
One of the most common questions patients ask is whether progesterone should be taken cyclically or continuously. There is a great deal of discussion about this online, with some sources suggesting that continuous progesterone is harmful. The clinical reality is more nuanced — the choice between cyclic and continuous progesterone depends primarily on life stage, ovulatory status, and individual response. It is a clinical decision, not an ideological one.
Reproductive Age
For women of reproductive age — those who are ovulating or who could naturally ovulate — cyclic progesterone is almost always the approach used. This is because continuous progesterone in this age range can actually make cycles less regular and may disrupt ovulation, rather than supporting it.
Cyclic progesterone, by contrast, allows for natural ovulation to continue. In patients with polycystic ovary syndrome, cyclic progesterone can even encourage the return of natural ovulation over time. It does this indirectly, by lowering testosterone levels that would otherwise block ovulatory function.
Perimenopause
In perimenopause, the ovaries are still producing estrogen — often in fluctuating amounts. Cyclic progesterone is generally used during this phase because giving progesterone continuously while there is any remaining cycle regularity can make cycles more irregular.
As perimenopause progresses and cycles become highly irregular or infrequent, the choice between cyclic and continuous becomes more open. At this stage, some patients prefer cycling on and off, while others feel better with continuous use. This is individualized based on symptoms, preferences, and clinical response.
Menopause
After menopause, when cycles have stopped, the decision between cyclic and continuous progesterone is largely guided by patient preference and clinical goals. Some patients enjoy the calming effect of progesterone and prefer to take it continuously because they do not feel as well without it. Others prefer the on-and-off pattern of cycling.
One important consideration: cyclic progesterone in menopause is more likely to cause withdrawal bleeds when the progesterone is stopped each cycle. For some patients this is acceptable; for others it is a significant factor in choosing continuous use instead.
In all cases, we individualize treatment. We draw on clinical experience to determine a starting approach, and then adjust based on how each patient responds.
Whether cyclic or continuous progesterone is appropriate for you depends on your individual situation — including your age, cycle status, symptoms, and goals. Your practitioner can help determine the right approach after a thorough assessment. For more context on the safety profile of bioidentical hormones, see our article on bioidentical hormone therapy safety updates.
Side Effects and Risks of Cyclic Progesterone Therapy
Side effects of natural cyclic progesterone are rare as this hormone is naturally present in the body for 2 weeks out of every month. Natural progesterone has not been found to cause the same risks for blood clots as synthetic progestins have(5).
Natural progesterone can definitely cause sleepiness and for this reason, it is given at bedtime. In many cases, progesterone can cause some mild side effects initially such as menstrual spotting during the first cycle of use in particular. This is more common in patients with high levels of estrogen and typically resolves after the first cycle.
Since progesterone works slowly over several cycles, most side effects are mild and resolve as treatment continues. Although there are some patients who can’t tolerate progesterone, this is quite rare due to its natural presence in such large quantities in the body when hormones are regulated.
Cyclic progesterone can be an extremely helpful treatment for PMS – Premenstrual Syndrome and depressive, irritable or anxious mood changes that occur before the period arrives
For a related but different and more serious condition. PMDD – Premenstrual Dysphoric Disorder, progesterone is not always a good choice.
PMDD is a serious hormone-related change in mental health and functionality that affects a patient’s ability to function in their daily life. Even when hormones are perfectly balanced, patients with PMDD have a different brain/mood response to hormone changes than those without the condition. Patients with PMDD may not be able to tolerate progesterone, other hormone treatments and their own natural ovulatory hormonal changes.
What to Expect When Starting Cyclic Progesterone
When first starting progesterone, the calming and sedating effects can feel stronger for the first few days. This is normal and typically settles as the body adjusts. Most patients tolerate progesterone well after this brief initial period.
How quickly patients notice changes depends on the condition being addressed:
- Sleep and mood: These are often the quickest symptoms to respond. Many patients notice improvements within the first few days of use, after the initial adjustment period.
- Heavy periods: Lightening of menstrual flow is commonly observed within the first couple of months. More significant changes typically occur by 3–4 months. The first cycle may still be irregular, with additional shedding as the thickened uterine lining clears.
- PCOS cycle regulation: Improvements in cycle regularity are often seen within the first couple of cycles. Consistent, predictable monthly cycles typically develop within 6–9 months of treatment.
Individual timelines vary based on your specific condition, health history, and treatment approach. Your practitioner will monitor progress and adjust as needed.
Frequently Asked Questions
What is cyclic progesterone therapy?
Cyclic progesterone therapy involves taking natural progesterone for 14 days “off” and 14 days “on” repeatedly. This can be completed with micronized progesterone, or natural progesterone vaginal suppositories.
When should I take cyclic progesterone?
Cyclic progesterone is always prescribed and monitored by a doctor or naturopathic doctor with prescribing rights. It is always taken at bedtime, since it can cause sleepiness. Taking it at bedtime can also improve sleep quality, allowing patients to experience better, deeper sleep.
How do you get prescribed cyclic progesterone?
At White Lotus, we commonly prescribe cyclic progesterone therapy as micronized progesterone suppositories. If you are located in Ontario, reach out to us to book an appointment either in-person or through telemedicine. We often complete lab testing before prescribing this treatment so we can track the progress of our patients.
Cyclic progesterone therapy is one component of a comprehensive approach to PCOS care. For a full overview of how we assess and manage PCOS — including when cyclic progesterone is appropriate — see how we approach PCOS care at our Toronto clinic.
How does cyclic progesterone induce periods or bleeds?
Cyclic progesterone can induce withdrawal bleeds for patients with PCOS who do not ovulate. It opposes the effect of estrogen on the lining and when it is stopped, the lining will shed. This is important to prevent thickening of the linining (endometrial hyperplasia) and reduces the risk of endometrial cancer.
Cyclic progesterone can also reduce levels of androgens like testosterone in PCOS. Since androgens block ovulation, this can allow some patients to ovulate naturally and have natural periods when the 14 days “on” is complete.
Is cyclic progesterone therapy safe?
Natural cyclic progesterone or micronized progesterone is generally a safe and well-tolerated treatment. Our bodies should have a large amount of progesterone in them for 14 days out of every 28 days. In patients with PCOS who don’t have periods, cyclic progesterone can induce bleeds and reduce the risk of endometrial hyperplasia (thickening of the lining)
Keep in mind, that natural progesterone is different from synthetic progestins. Progesins have various side effects and risks depending on the category and type. It is always important to confirm which type of progesterone is being prescribed.
When should I take progesterone for perimenopause?
In perimenopause, cyclic progesterone is typically prescribed while menstrual cycles are still occurring — even if they have become irregular. Your practitioner determines the appropriate timing based on your current cycle patterns, symptoms, and hormone levels. Progesterone is always taken at bedtime, as it has a natural calming effect that supports sleep. The specific days of your cycle on which progesterone is taken are individualized to your situation. If you are experiencing perimenopause symptoms and are interested in a comprehensive assessment, learn more about our menopause and perimenopause program.
Do I have to take cyclic progesterone forever?
No. Cyclic progesterone therapy is typically prescribed for a minimum of approximately nine months, though the duration depends on the condition being treated and your individual response. When patients are ready to discontinue, there are several approaches your practitioner can use, depending on your treatment and goals.
Some patients find that they prefer to continue progesterone long-term because they feel better with it than without it — and it is considered safe to continue with ongoing practitioner oversight. For patients with PCOS, in some cases the condition can show lasting improvement after a sustained course of treatment, and progesterone may no longer be needed. Your practitioner will discuss timing and approach with you throughout your care.
Can cyclic progesterone cause cancer or weight gain?
These are common concerns, and it is important to distinguish natural micronized progesterone from synthetic progestins — they have different safety profiles. Research has not found natural progesterone to carry the same risks for blood clots that have been associated with synthetic progestins.
Regarding cancer risk: cyclic progesterone actually helps protect against endometrial hyperplasia — a thickening of the uterine lining that, if left unchecked, can increase the risk of endometrial cancer. By inducing regular withdrawal bleeds, cyclic progesterone prevents this buildup. Weight gain is a common concern but is not a typical clinical observation with natural micronized progesterone. For a broader discussion of bioidentical hormone safety, see our article on bioidentical hormone therapy safety updates.
Is natural progesterone the same as birth control?
No. Natural micronized progesterone is chemically identical to the progesterone your body produces after ovulation. Birth control pills and hormonal IUDs contain synthetic progestins, which are structurally different molecules with different effects and risk profiles. Many patients who come to our clinic have previously used synthetic progestins and are surprised to find that natural progesterone is a very different experience. The distinction between natural progesterone and synthetic progestins is one of the most important and most commonly misunderstood aspects of hormonal therapy.
How long does cyclic progesterone take to work?
This depends on the condition being treated. Sleep and mood tend to respond the most quickly — many patients notice improvements within the first few days of starting progesterone, after a brief initial adjustment period. For heavy periods, lightening of menstrual flow is often noticed within the first couple of months, with more significant changes typically occurring by three to four months. For PCOS cycle regulation, improvements in regularity are often seen within the first couple of cycles, with consistent monthly cycles typically developing within six to nine months. Individual timelines vary, and your practitioner will monitor your progress throughout treatment.
What Happens at Your First Visit
Your first visit begins with a comprehensive review of your health history — including your menstrual and hormonal history, any previous hormone testing, thyroid health, iron status, and overall wellness. Your practitioner will then arrange relevant lab testing, which commonly includes hormone levels, thyroid function, and iron studies, among other markers appropriate to your situation.
Based on this assessment, your practitioner will discuss whether cyclic progesterone is appropriate for you, what the treatment would involve, and what to expect. The first visit is exploratory — it is an opportunity to ask questions and understand your options, not a commitment to any particular treatment.
In Ontario? Come see us...
White Lotus Clinic is located in North York, Toronto. In-person appointments are available at our clinic for patients in the Toronto area Virtual and phone appointments are available to patients anywhere in Ontario.
Your first visit is exploratory to review your history, symptoms, and lab results — not a commitment to continued treatment. Read more about our Naturopathic PCOS program.
For patients experiencing perimenopause or menopause symptoms, cyclic progesterone may be one component of a broader treatment approach. Learn more about our menopause and perimenopause program.
References
- The central role of ovulatory disturbances in the etiology of androgenic polycystic ovary syndrome (PCOS)—Evidence for treatment with cyclic progesterone
- Inflammatory Markers in Dysmenorrhea and Therapeutic Options
- Progesterone Alleviates Endometriosis via Inhibition of Uterine Cell Proliferation, Inflammation and Angiogenesis in an Immunocompetent Mouse Model
- Progesterone Is Essential for Protecting against LPS-Induced Pregnancy Loss. LIF as a Potential Mediator of the Anti-inflammatory Effect of Progesterone
- Use of hormone replacement therapy and risk of venous thromboembolism: nested case-control studies using the QResearch and CPRD databases


